Arthritis of the Basilar Joint of the Thumb
Arthritis literally translated from the Latin means joint inflammation. It can have different forms, the most common being “wear and tear” or osteoarthritis, post-traumatic arthritis from prior injury or fracture, and rheumatoid arthritis which is a body-wide genetic affliction.
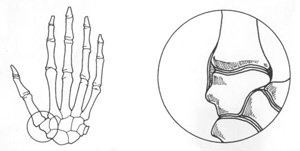 In a normal human joint, bone ends are covered by a smooth layer of cartilage,
and the joint is bathed
in lubricating synovial fluid. In advanced arthritis, the cartilage layer is thin or absent.
The joints become inflamed. Friction from worn out joint surfaces combined with inflammation causes pain.
The joint at
In a normal human joint, bone ends are covered by a smooth layer of cartilage,
and the joint is bathed
in lubricating synovial fluid. In advanced arthritis, the cartilage layer is thin or absent.
The joints become inflamed. Friction from worn out joint surfaces combined with inflammation causes pain.
The joint at
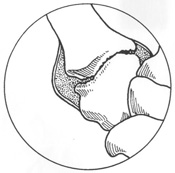 the base of the thumb (the basilar joint) is very susceptible to arthritis.
This is partly because of its large range of motion.
If patients have loose ligaments, mobility is increased even more and may lead to an increased incidence of
arthritis. It is much more common in women than men, since women are more likely to have loose ligaments.
the base of the thumb (the basilar joint) is very susceptible to arthritis.
This is partly because of its large range of motion.
If patients have loose ligaments, mobility is increased even more and may lead to an increased incidence of
arthritis. It is much more common in women than men, since women are more likely to have loose ligaments.
Signs and Symptoms
Any activities requiring forceful use of the thumb may be quite painful. Strength decreases. Opening jars and door knobs becomes difficult. Eventually, any thumb motion becomes difficult. It may become difficult to bring the thumb away from the palm of the hand. Adjacent joints may become deformed to compensate for the limited motion at the thumb joint.
Patients complain of pain at the base of the thumb, and the joint may be tender. Sometimes swelling is evident at the joint. Manipulation of the first metacarpal may be painful.
Treatment
Splinting the thumb joint in a stable position to rest it can be effective in eliminating the symptoms of arthritis. Local injection of steroid medication into the joint can relieve symptoms temporarily or on occasion permanently.
If these conservative treatment methods fail, surgical reconstruction of the joint may be warranted. By removing the diseased joint and replacing it with other material, pain can be relieved and function restored. Parts of the bony surfaces of the basilar joint are removed. The procedure is generally done as an outpatient.
After surgery a dressing will be applied to your hand, and a wire may be used to hold the thumb in position while the soft tissues heal. It is very important that you elevate the hand and keep the fingers moving after surgery to prevent swelling and stiffness. The dressing will be removed one to two weeks after surgery. Depending on the particular type of procedure performed, immobilization may be continued up to six weeks after surgery. At this point, exercises will be initiated to restore range of motion of the thumb, under the direction of hand therapists. Splints will be constructed for you and must be worn while healing progresses.